Key Summary: This study examined the relationship between heart rate variability (HRV) measured at hospital admission and symptom remission at discharge in first-episode psychosis patients. Among HRV measures at admission, patients who showed lower high-frequency (HF) power and a faster heart rate decline trend (BPM slope) were more likely to respond well to treatment and achieve remission. These findings suggest that HRV, a low-cost physiological measure, has potential to inform early psychosis treatment strategies.
1. Study Background and Objectives
Psychosis is a serious mental health condition with high global prevalence, commonly beginning in young adulthood and accompanied by suicide risk and various comorbidities. Even among treated first-episode patients, the remission rate is only 58%, the complete recovery rate just 38%, and only 29% receive appropriate treatment.
Previously, demographic factors such as age, sex, and symptom severity, along with neurophysiological biomarkers like neuroimaging, were used to predict prognosis, but these methods had limitations due to high cost and lack of practicality.
Heart rate variability (HRV) has emerged as a promising alternative. HRV measures the variability in time intervals between heartbeats, reflecting the regulatory capacity of the autonomic nervous system and overall health status. Higher HRV indicates good autonomic nervous system adaptation, while lower HRV indicates functional decline and disease risk.
"Heart rate variability is a non-invasive marker of autonomic nervous system activity that holds promise as a low-cost prognostic biomarker in psychosis."
The purpose of this study was to determine, in a real-world clinical setting, whether autonomic patterns measured by HRV at admission in first-episode psychosis patients are associated with symptom remission at discharge.
2. Study Design and Methods
Participants and Data Collection
- Subjects: 78 suspected first-episode psychosis patients (mean age 30.8, 45% female) admitted to the Psychiatric University Hospital of Zurich between 2018 and 2024
- Diagnostic criteria: Various psychosis diagnoses including schizophrenia spectrum (F2)
- HRV measurement: 2-minute resting-state electrocardiogram (ECG) at admission
- Clinical assessments:
- Clinical Global Impression - Severity (CGI-S)
- Health of the Nation Outcome Scales (HoNOS)
- Classification as "remission" or "partial/non-remission" based on clinician assessment at discharge
HRV Analysis Procedure
- Analysis measures:
- High-frequency (HF) power and low-frequency (LF) power (both log-transformed)
- Mean BPM
- BPM slope (slope of heart rate change over time)
- Other:
- ECG data quality verification and application of international standard protocols
Data Analysis
- Statistical methods:
- Interval-based means, sex comparisons
- Binomial logistic regression with 5-fold cross-validation for predictive evaluation
- Interpretation centered on predictive performance (AUC)
"In the prediction model, only log(HF) and BPM slope were significantly associated with remission status."
3. Key Results
Patient Characteristics Summary
- Mean age: 30.8 years, male-to-female ratio 55:45
- At discharge, 33.3% of patients (26) achieved remission, while the remaining 66.7% (52) were in partial/non-remission
- No significant differences in sex, medication type (olanzapine, risperidone, aripiprazole, etc.), number of medications, or clinical indicators
- Primary diagnoses: schizophrenia (27%), acute and transient psychotic disorder (41%), schizoaffective disorder, and others
HRV and Remission Prediction
- In the initial model (including all 4 ECG variables):
- Only log(HF) and BPM slope were significant
- In the final model (including only log(HF) and BPM slope):
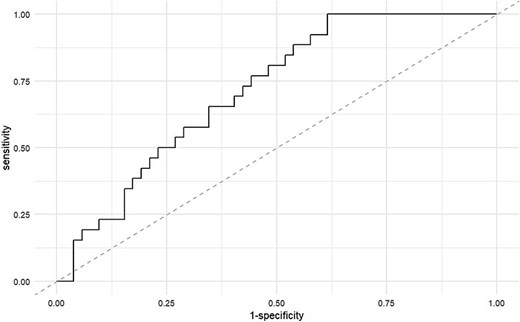
- Prediction accuracy (AUC) was 0.714, indicating above-moderate predictive power
- Remission group:
- Lower HF (high-frequency) power and more pronounced BPM slope (heart rate decline trend)
- That is, patients whose parasympathetic activation (rest/relaxation) was not excessive at admission and whose heart rate stabilized quickly showed better treatment responses
"Lower HF power and faster BPM decline at admission increased the probability of remission."

4. Discussion and Clinical Interpretation
The study found that lower HF and faster BPM decline at admission were associated with remission at discharge. This suggests that "autonomic flexibility" plays an important role in treatment responsiveness.
"Intuitively, higher HRV (especially HF) is considered healthier, but in this study, lower HF was more associated with predicting remission."
This indicates that rather than patients being "locked into" a relaxation and energy-conservation mode (parasympathetic dominance) with high HF, patients whose nervous system is more flexible in transitioning between tension and relaxation can better adapt to psychological and physical stress and respond better to treatment.
Similarly, in existing research on anxiety disorders and depression, cases where lower HRV is associated with better prognosis have been reported, supporting the recent research trend that the clinical meaning of HRV can vary depending on context and diagnosis.
Additionally, an important implication is that these HRV markers may reflect the difference between state and trait -- distinguishing "treatment responsiveness" rather than "symptom severity."
"These results propose the role of HRV as a predictor of remission and provide evidence for early treatment strategies and personalized care."
5. Limitations and Future Directions
This study has limitations inherent to its observational, retrospective design, preventing clear causal conclusions. Several factors were not fully controlled, including medication effects at the time of ECG measurement, sex, other health conditions (cardiac disease, respiratory function, etc.), and inconsistency of interventions. Additionally, the 2-minute ECG measurement was relatively short, repeat measurement at discharge was not performed, and respiratory data as well as time-domain HRV measures (RMSSD, SDNN, etc.) were absent.
However, HRV clearly has the strengths of being cost-effective, easy to apply, and readily usable in clinical settings.
6. Clinical and Research Implications
- This study demonstrated that simple physiological measures (HRV) can predict treatment outcomes.
- Notably, HRV should be interpreted not as a single value, but as a combination of multiple indicators and their temporal changes.
- Future studies should aim to improve predictive power and expand personalized treatment applications through larger prospective studies, repeated HRV measurements, and integrated analysis with respiratory, behavioral, and clinical indicators.
Conclusion
This study presented the practical possibility that early treatment outcomes and remission potential can be predicted through simple HRV measurement in first-episode psychosis patients. HRV is attracting attention as a new biomarker for establishing personalized clinical treatment strategies, and broader research and real-world clinical application are anticipated in the future.
"In the future, integrated analysis of HRV with clinical, behavioral, and digital biomarkers will enable more precise prediction and personalized treatment."